'' The Life Changing Effects of a Prolapsed Lumbar Disc ''
An Employer's Manual Handling Risk Management Responsibility
Written by Gareth Milner BSc (Hons) Ost.
10 Minute Read

Firstly let’s take a brief look at a Spinal Disc’s structure and function. The spinal discs are made of cartilage and are sandwiched between each pair of vertebrae. They are shock absorbers and give the spine flexibility. The thickest disc is between the 5th lumbar vertebrae and the sacrum (L5/S1 disc).
This disc is the most commonly injured, followed by the L4/L5 disc and the C5/C6, C6/C7 discs i.e. the lower back and the lower neck. Each disc is composed of an annulus fibrosis and a nucleus pulposus (shown in the image below right).
The annulus (or outer portion) is made up of around 20 layers of tough, fibrous tissue (similar to the layers of an onion) which holds the inner nucleus in place. The nucleus is 80% water and is a more gel-like substance. As long as the outer annulus is undamaged, the nucleus will keep the vertebrae apart.
The discs are rather like a balloon filled with water being squeezed between two records. When you bend your back the vertebrae squeeze one end of the disc, shifting the gel interior to one side. The other end of the disc is stretched and bulges outwards.




What happens when a Disc Prolapses?

Disc injuries are most common between the ages of 35 to 45 when the discs are full of the gel-like nucleus. A common medical term for a disc injury is a ‘slipped disc’. However its name is very misleading as the disc is not displaced in any way. The outer one third of the annulus fibrosis receives pain sensitive nerve endings and will detect damage. In a Disc Herniation, the outer rear layers of the annulus weaken and the gel-like nucleus protrudes to the rear. Affecting the L5/S1 disc, this would cause daily symptoms of aching in the lower back and buttocks. Pain will continue down one or both legs to the foot, perceived as an ache or burning, with pins and needles and numbness in the foot.
In a Disc Prolapse, the annulus tears and the gel-like substance extrudes posteriorly compressing the spinal cord and spinal nerves. Pain is severe and sharp in all ranges of movement (especially forward bending) with accompanying back muscle spasm. Affecting the L5/S1 disc, pain will shoot down one or both legs which is called ‘Sciatica’. The MRI Scan (shown above) details a prolapse in the patient at their L5/S1 level.

What are Risk Factors for a Disc Prolapse?
There are genetic factors related with Disc Prolapses. These could be on a cellular level with inherited weaknesses in connective tissues and collagen formation, leading to joints with reduced stability. There could be bony genetic factors that create biomechanically impaired lumbo-pelvic mechanics leading to abnormal strains on the L5/S1 disc. A poor diet is a major factor. Insufficient or poor quality protein intake would be one. Not drinking enough water is another, leading to discs that are less able to absorb compressive forces.
Smoking has been found to increase the likelihood of disc injury. Ergonomically, if you sit for hours at a desk everyday with work, especially with a desk set up that promotes poor spinal posture, including the overuse of a laptop, this will aggravate the lumbar discs. The same also goes for long and repetitive periods of driving. Obesity and having a sedentary lifestyle are major risk factors as loading the lumbar discs from above with excessive bodyweight will weaken the outer layer of the disc as the internal nucleus is forced against it. Excessive weight training, especially with the performance of Dead Lifting will promote a disc prolapse. Trauma from accidents are another cause. This could be from falls (from standing, off a horse or a bike, RTAs, sporting accidents etc.).

In writing my Book Sorry! We’re Closed (pictured to the left) I met and interviewed 7 people who suffered a considerable musculoskeletal injury from their manual handling tasks and who were each successful in their claim for damages. ‘Mr. Goddard’ was employed by ‘Fine Ships Ltd’ . The task that initiated his prolapsed lumbar disc involved lowering a 30kg engine part into the engine compartment. It involved kneeling on both knees and forward bending to lower the engine part below the level of the yacht’s rear platform floor (you can see the Book's illustration of this task in the image gallery to the left). ‘Mr. Goddard’ was awarded in Court the sum of £160, 980.
What Manual Handling Practices can cause a Disc Prolapse?
Lifting with a forward bend and twist is the main culprit. When forward bending is coupled with a twist there is further stretching of the disc annulus and further micro-trauma. This is a more hazardous movement for the spine than forward bending alone. Below are some real life tasks that over time will wear down the L5/S1 disc. Another hazardous practice is pulling using one arm and bodyweight, just like how most people pull a palletised load. Or in the Food Industry Operatives commonly pull cages using both hands leaning towards where they are pulling it. However any Manual Handling hazardous practice that is repetitively performed, like carrying on the shoulder, pushing with an excessive forward bend and use of bodyweight, carrying long distances etc. will damage the discs and predispose to a prolapsed disc and/ or degenerative disc disease.
How is a Prolapsed Lumbar Disc diagnosed?
A prolapsed disc is very easy to clinically diagnose. As a practising Osteopath people (that could walk) would come to my clinic with extreme lower back pain that would be shooting down one, or both legs. They would hobble through the door into the clinic room and would be unable to sit down. The onset of injury commonly was from a lifting incident.
When the L5/ S1 disc prolapses there is huge compression on the sacral plexus of nerves in the spinal canal. This impairs the function of the nerves to the lower leg and feet. With this, Clinical Tests include the following:
-
Straight Leg Raise (shown below left)
-
Muscle Testing of Lower Leg Muscles (shown below middle)
-
Reflex Testing including the Achilles Heel Deep Tendon Reflex (shown below right)
-
Sensory Testing of the Lower Leg and Foot


With an L5/ S1 disc prolapse the Straight Leg Raise would elicit a shooting pain down the leg raised. There would be weakness in the lower leg muscles, a reduced or non-existent Achilles Tendon reflex and reduced sensation in the lower leg and/ or foot. With the onset of injury, location of the pain (including sciatica) and these clinical findings this is well sufficient to diagnose a Prolapsed L5/ S1 Disc.

Immediately after the incident that initiated the prolapse, pain in the lower back and down the leg (or both) is extreme. Typically an ambulance would be needed to take the person to hospital. A Clinical Assessment would be made by a Neurologist to determine whether there is compression of nerves to the bladder. If there was surgery would be performed as a matter of urgence. The definitive diagnosis would be made at a hospital via a MRI Scan.
What Disability does a Prolapsed Lumbar Disc cause?
Immediately after the incident that initiated the prolapse, in order to allow the person to walk and return home, the strongest painkillers would be given including morphine. At home maximum dosage of tramadol and naproxen would be needed to make the pain at least a little more bearable. The person will not be able to work and will be on sick pay.
Life with a prolapsed lumbar disc, whilst on a waiting list for surgery, make no mistake is miserable. Even though maximum dosages of painkillers are taken, pain in the lower back and sciatica will be intolerable. Simple life tasks like getting dressed, putting on your shoes, walking, driving, shopping etc. will all be physically very difficult with forward bent postures causing shooting pains in the lower back and down the legs. Sleep may also be affected, not only by the pain but through the side effects of the tramadol.
What can a Spinal Surgeon do?

Ideally surgery would be the next day after the disc has prolapsed. But unless there is bladder involvement (as mentioned above) the patient will be placed on a NHS waiting list. Of course, there are private options available but again there will be some waiting for the surgery date and at a significant personal financial cost in a Private Hospital.
In the past surgery was 'open' but these days it is commonly through keyhole surgery.
The immediate aim of the surgery is to take the compression off of the spinal cord and spinal nerve. This involves removal of part or the whole of the prolapsed disc. There can also be removal of bone from the vertebra, which again is to reduce compression on the spinal nerve by allowing more space. These days if the whole disc is removed, an artificial disc can be inserted. However this is still not that common.
Concerning the results of surgery, pain is generally significantly reduced as the compression on the spinal cord/ nerve has been removed. However there is significant swelling of the injured area as well as the muscle spasm that will take time to reduce following the initial prolapse accident. Make no mistake, surgery is not the answer to disc prolapses. The solution is to never get one in the first place. I have seen many patients who have said to me 'it's ok, I will be getting my back op soon!' Only to again be in crippling pain 2 years after the operation, and back on a waiting list to have another procedure. This is an extreme due to the sporting repetition, but just look at Tiger Woods.
In Summer 2026, I will be interviewing a Spinal Surgeon at a Podcast Studio. LinkedIn connect with me to be notified when this Podcast is available to watch.
What can an Osteopath do?
Just after the initial onset of the prolapse, there will be massive spasm of the lower back muscles and with the spinal cord/ nerve compression from the ruptured disc and swelling, the person will be in agony. At this stage, I will be honest, reducing the pain with Manual Therapy (be it Osteopathy, Chiropractic or Physiotherapy) will be near impossible, however if I had suffered this injury, I would still be consulting an Osteopath or a Chiropractor to reduce the back muscle spasm, at the very least. Treatment would be private and not paid for by the NHS. You can find a local Osteopath via this link to the Institute of Osteopathy website.
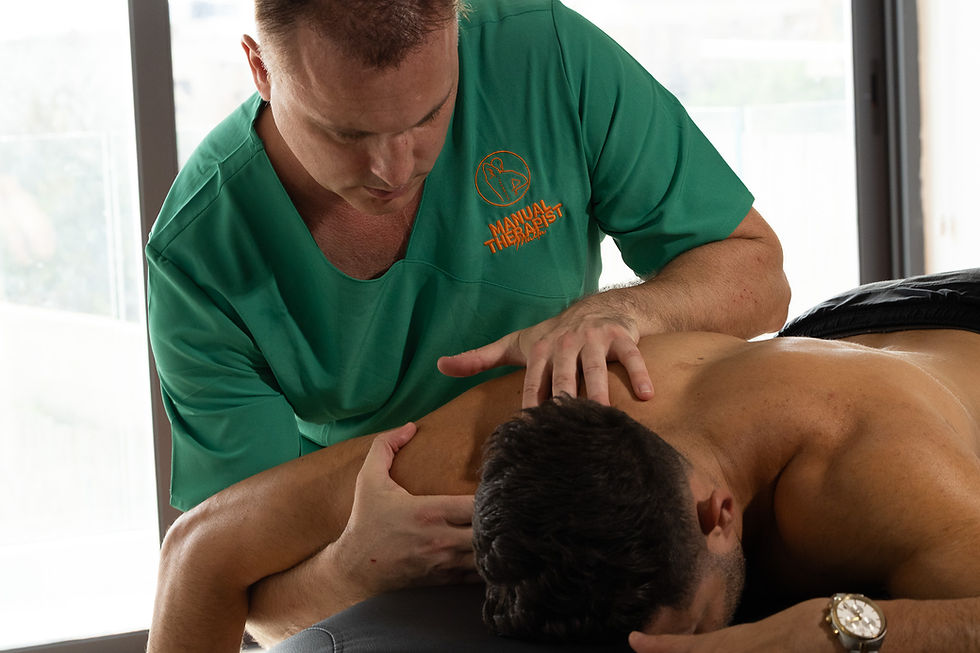



My approach to treating a patient who presents with the early stage of a prolapsed disc is the following. After Clinical Examination the patient is treated in the sidelying position, initially with Interferential Electrotherapy for 10 minutes. This raises the body's natural endorphin levels in the nerve pathways of the lower back. The application of soft tissue massage/ inhibition in the sidelying position would then be applied. With this the patient would be made more comfortable with a reduction in pain. Following this, the application of Craniosacral Technique to the lower back and pelvis would be performed, releasing the physical strain and realigning the L5/S1 vertebrae.
High Velocity Thrust Manipulation (the technique where the joint makes a CRACK sound) would NEVER be performed with such a clinical presentation. Thrust manipulation is a perfectly safe and effective joint mobilisation technique, in but in the right clinical presentation and of course in an Osteopath or Chiropractors' professionally trained hands. The above treatment protocol would be performed over 5 weeks with 2 appointments needed each week. Through this time patients would be on high dose tramadol and naproxen. The application of an Ice Pack 2-3 times daily would also be indicated.
Once surgery has been performed Manual Therapy is indicated to restore the lower back into good alignment and function. Osteopathic Manipulative Therapy would support the healing of the injury, and reduce the physical disability that the prolapse has caused. Through this period the patient would need to perform daily rehabilitative exercises to support the improvement in their situation.
Business Loss - The Injury at Work Claim & The Legal Shark



The above illustrations by Emma Farrell feature in my Book Sorry We're Closed. They detail the Legal Shark, sitting at his desk looking all sharky; lying in wait for the Business Owner's hard earnt money; and biting the Business Owner's arse. At the bottom of this page you can click the blue tab to read Tip 4 - Beware the Legal Shark from Sorry We're Closed.
Legal Sharks are desperate to get their teeth into Injury at Work Claims and a person suffering a prolapsed disc at work ... is their holy grail. If a Legal Shark can prove that the person's prolapse was due to their Manual Handling tasks, and if this was accompanied by a lack of evidence of the person receiving Manual Handling Training then it's successful Claim Time Baby! Click on the LegalExpert.co.uk image to the right where you will have some uncomfortable reading on possible claim payouts. Ouch!
My Conclusion

This Blog Post included the words 'An Employer's Manual Handling Risk Management Responsibility'. Prolapsed Discs ruin lives. The disability will be huge. The person's misery will be huge. The dangers of surgery exist. The lack of surgical success exists. £160,000 payouts exist.
Health & Safety Managers and Business Owners have a responsibility to make sure that their Employees, under their watch, do NOT suffer this injury at work. Of course people do things outside of work that create strain and disc injuries. But with the amount of hours people perform
their repetitive Manual Handling tasks, week in week out, the majority of the blame will lie with their job. Through detailed Manual Handling Risk Assessment and actioned Risk Reduction Solutions; changing habits for the better within your Workforce through Expert delivered 'in the working environment' Manual Handling Training, supported by Digital Training, the risk of a Lumbar Disc Prolapse within your workforce will be as low as you can get it.

Essay 4 - Beware the Legal Shark
.jpg)
An Osteopathic Treatment for Lower Back Pain

BackCare
Q&As
.jpg)
.jpg)




